Below you will find the list of references that are used in this fact sheet. All sources used can be consulted or retrieved via our Library portal. Here you can also find more literature on this subject.
[1]. Davidse, R.J., Vlakveld, W.P., Doumen, M.J.A. & Craen, S. de (2010). Statusonderkenning, risico-onderkenning en kalibratie bij verkeersdeelnemers. Een literatuurstudie [State awareness, risk awareness of and calibration by road users: A literature study]. R-2010-2 [Summary in English]. SWOV, Leidschendam.
[2]. WHO (2016). Drug use and road safety. A policy brief. World Health Organization, Geneva.
[3]. Wolff, K., Brimblecombe, R., Forfar, J.C., Forrest, A.R., et al. (2013). Driving under the influence of drugs. Report from the expert panel on drug driving. UK Department for Transport, London.
[4]. Couper, F.J. & Logan, B.K. (2014). Drugs and human performance fact sheets. Report No. DOT HS 809 725. National Highway Traffic Safety Administration (NHTSA), Washington.
[5]. Bredewoud, R.A. (2009). Rijgevaarlijke geneesmiddelen: eindelijk duidelijkheid? CBR, Rijswijk.
[6]. Faber, E., Brons, M., Bruring, D.P., Hamelijnck, M.A.F., et al. (2016). LESA Geneesmiddelen en Verkeersveiligheid. Nederlands Huisartsen Genootschap NHG, Utrecht.
[7]. Croes, E., Meijer, H., Van Dort, B., Remmits, J., et al. (2018). Factsheet GHB. AF1656, December 2018. Trimbos-instituut, Utrecht.
[8]. Van Miltenburg, C., Van Laar, M. & Van Goor, M. (2019). Factsheet Ketamine. AF1708. Trimbos-instituut, Utrecht.
[9]. Van Goor, M. (2018). Factsheet Lachgas. Update maart 2018, AF1384. Trimbos-instituut, Utrecht.
[10]. Giorgetti, R., Marcotulli, D., Tagliabracci, A. & Schifano, F. (2015). Effects of ketamine on psychomotor, sensory and cognitive functions relevant for driving ability. In: Forensic Science International, vol. 252, p. 127-142.
[11]. Coull, J.T., Morgan, H., Cambridge, V.C., Moore, J.W., et al. (2011). Ketamine perturbs perception of the flow of time in healthy volunteers. In: Psychopharmacology (Berl), vol. 218, nr. 3, p. 543-556.
[12]. Liakoni, E., Dempsey, D.A., Meyers, M., Murphy, N.G., et al. (2018). Effect of gamma-hydroxybutyrate (GHB) on driving as measured by a driving simulator. In: Psychopharmacology (Berl), vol. 235, nr. 11, p. 3223-3232.
[13]. Houwing, S., Hagenzieker, M., Mathijssen, R., Bernhoft, I.M., et al. (2011). Prevalence of alcohol and other psychoactive substances in drivers in general traffic; Part II: Country reports. Deliverable D2.2.3 Part 2 of the EU FP6 project DRUID. European Commission, Brussels.
[14]. Vias institute (2019). Country fact sheet Netherlands. ESRA2_2018 survey (E-Survey of Road users'Attitudes). Vias institute, Brussels, Belgium.
[15]. Politie (2018). In jaar tijd 1250 keer drugs in het verkeer. Politie, Den Haag. Retrieved on 19-03-2020 at www.politie.nl/nieuws/2018/september/28/00-in-jaar-tijd-1250-keer-drugs-in-het-verkeer.html .
[16]. Trimbos-instituut (2020). Cijfers drugs: gebruik en trends. Trimbos-instituut, Utrecht. Retrieved on 28-01-2020 at www.trimbos.nl/kennis/cijfers/cijfers-drugs#sub6982.
[17]. Giele, T. (2018). Ook één pilletje is al te veel achter het stuur. Provinciale Zeeuwse Courant. Retrieved on 28-01-2020 at www.pzc.nl/zeeuws-nieuws/ook-een-pilletje-is-al-te-veel-achter-het-stuur~aba1bd04/.
[18]. Van Laar, M.W. & Van Gestel, B. (red.) (2019). Nationale Drug Monitor NDM: Jaarbericht 2018. Wetenschappelijk Onderzoek en Documentatiecentrum WODC / Trimbos-instituut, Den Haag / Utrecht.
[19]. Lemmens, L.C. & Weda, M. (2013). Polyfarmacie bij kwetsbare ouderen Inventarisatie van risico’s en mogelijke interventiestrategieën. RIVM briefrapport 080027001/2013. RIVM.
[20]. LeRoy, A.A. & Morse, L.M. (2008). Multiple medications and vehicle crashes: analysis of databases. U.S. Department of Transportation, National Highway Traffic Safety Administration (NHTSA), Washington.
[21]. Isalberti, C., Van der Linden, T., Legrand, S.-A., Verstraete, A., et al. (2011). Prevalence of alcohol and other psychoactive substances in injured and killed drivers. Deliverable D2.2.5 of the EU FP6 project DRUID. European Commission, Brussels.
[22]. RUG, NFI & SWOV (2012). Jaarlijks 33 tot 66 verkeersdoden door rijgevaarlijke geneesmiddelen. Gezamenlijk persbericht van de Rijksuniversiteit Groningen (RUG), Nederlands Forensisch Instituut (NFI) en de Stichting Wetenschappelijk Onderzoek Verkeersveiligheid (SWOV). Retrieved on 19-06-2019 at www.rug.nl/news/2012/05/065_12degier.
[23]. Elvik, R. (2013). Risk of road accident associated with the use of drugs: A systematic review and meta-analysis of evidence from epidemiological studies. In: Accident Analysis & Prevention, vol. 60, p. 254-267.
[24]. Rogeberg, O. & Elvik, R. (2016). The effects of cannabis intoxication on motor vehicle collision revisited and revised. In: Addiction, vol. 111, nr. 8, p. 1348-1359.
[25]. Els, C., Jackson, T.D., Tsuyuki, R.T., Aidoo, H., et al. (2019). Impact of cannabis use on road traffic collisions and safety at work: Systematic review and meta-analysis. In: Canadian Journal of Addiction, vol. 10, nr. 1, p. 8-15.
[26]. Rogeberg, O. (2019). A meta-analysis of the crash risk of cannabis-positive drivers in culpability studies—Avoiding interpretational bias. In: Accident Analysis & Prevention, vol. 123, p. 69-78.
[27]. Hels, T., Bernhoft, I.M., Lyckegaard, A., Houwing, S., et al. (2011). Risk of injury by driving with alcohol and other drugs. Deliverable D2.3.5 of the EU FP6 project DRUID. European Commission, Brussels.
[28]. Martin, J.P., Sexton, B.F., Saunders, B.P. & Atkin, W.S. (2000). Inhaled patient-administered nitrous oxide/oxygen mixture does not impair driving ability when used as analgesia during screening flexible sigmoidoscopy. In: Gastrointestinal endoscopy, vol. 51, nr. 6, p. 701-703.
[29]. Sinclair, D.R., Chung, F. & Smiley, A. (2003). General anesthesia does not impair simulator driving skills in volunteers in the immediate recovery period - a pilot study. In: Canadian journal of anaesthesia, vol. 50, nr. 3, p. 238-245.
[30]. Garakani, A., Jaffe, R.J., Savla, D., Welch, A.K., et al. (2016). Neurologic, psychiatric, and other medical manifestations of nitrous oxide abuse: A systematic review of the case literature. In: The American journal on addictions, vol. 25, nr. 5, p. 358-369.
[31]. Randhawa, G. & Bodenham, A. (2016). The increasing recreational use of nitrous oxide: history revisited. In: British journal of anaesthesia, vol. 116, nr. 3, p. 321-324.
[32]. Trojan, J., Saunders, B.P., Woloshynowych, M., Debinsky, H.S., et al. (1997). Immediate recovery of psychomotor function after patient-administered nitrous oxide/oxygen inhalation for colonoscopyv. In: Endoscopy, vol. 29, nr. 1, p. 17-22.
[33]. Rijksoverheid (2019). Blokhuis verbiedt lachgas door plaatsing onder Opiumwet. Rijksoverheid, Ministerie van Volksgezondheid, Welzijn en Sport. Retrieved on 26-02-2020 at www.rijksoverheid.nl/actueel/nieuws/2019/12/09/blokhuis-verbiedt-lachgas-door-plaatsing-onder-opiumwet.
[34]. CAM (2019). Risicobeoordeling lachgas. Coördinatiepunt Assessment en Monitoring nieuwe drugs CAM, Bilthoven.
[35]. Chihuri, S. & Li, G. (2017). Use of prescription opioids and motor vehicle crashes: A meta analysis. In: Accident Analysis & Prevention, vol. 109, p. 123-131.
[36]. Rudisill, T.M., Zhu, M., Kelley, G.A., Pilkerton, C., et al. (2016). Medication use and the risk of motor vehicle collisions among licensed drivers: A systematic review. In: Accident Analysis & Prevention, vol. 96, p. 255-270.
[37]. Leblud, J., Meesmann, U., Houwing, S. & Opdenakker, E. (2019). Themadossier Verkeersveiligheid nr. 4 Drugs en geneesmiddelen. Vias institute – Kenniscentrum Verkeersveiligheid, Brussel.
[38]. Goossens, F.X., Hasselt, N.E. Van & Sannen, A.M.L. (2012). Verslaving: Maatschappelijke gevolgen. Trimbos-instituut, Utrecht.
[39]. Nederlandse Vereniging voor Klinische Geriatrie (2019). Geneesmiddelen bij ouderen. Retrieved on 06-05-2019 at www.nvkg.nl/publiek/ziektebeelden/geneesmiddelen-bij-ouderen.
[40]. Artime, E., Qizilbash, N., Garrido-Estepa, M., Vora, P., et al. (2019). Are risk minimization measures for approved drugs in Europe effective? A systematic review. In: Expert Opinion on Drug Safety, vol. 18, nr. 5, p. 443-454.
[41]. Vervloet, M., De Jong, J. & Van Dijk, L. (2007). Rijgevaarlijke geneesmiddelen en verkeersdeelname: meningen van consumenten en professionals. Nivel, Utrecht.
[42]. Ziemerink, L. (2018). Drugsgebruik in het verkeer. TeamAlert, Utrecht.
[43]. TeamAlert (2018). Drugsgebruik achter het stuur. Rapportage doelgroepsanalyse. TeamAlert, Utrecht.
[44]. Weinstein, N.D. (1989). Optimistic biases about personal risks. In: Science, vol. 246, nr. 4935, p. 1232-1233.
[45]. Tyler, T.R. & Cook, F.L. (1984). The mass media and judgments of risk: Distinguishing impact on personal and societal level judgments. In: Journal of Personality and Social Psychology, vol. 47, p. 693-708.
[46]. Velthuijsen, A.S. (1996). Persoonlijke en onpersoonlijke impact van massamedia op risico-oordelen. PhD Thesis Universiteit van Amsterdam. Amsterdam.
[47]. Sargent-Cox, K.A., Windsor, T., Walker, J. & Anstey, K.J. (2011). Health literacy of older drivers and the importance of health experience for self-regulation of driving behaviour. In: Accident Analysis & Prevention, vol. 43, nr. 3, p. 898-905.
[48]. Orriols, L., Luxcey, A., Contrand, B., Gadegbeku, B., et al. (2016). Road traffic crash risk associated with benzodiazepine and z-hypnotic use after implementation of a colour-graded pictogram: a responsibility study. In: British journal of clinical pharmacology, vol. 82, nr. 6, p. 1625-1635.
[49]. Veisten, K., Houwing, S. & Mathijssen, R. (2010). Cost-benefit analysis of drug driving enforcement by the police. Deliverable D3.3.1 of the EU FP6 project DRUID. European Commission, Brussels.
[50]. Schulze, H., Schumacher, M., Urmeew, R. & Auerbach, K. (2012). Final Report: Work performed, main results and recommendations. DRUID Deliverable 0.1.8. BASt, Begisch Gladbach.
[51]. Davis, J.L.A. & Cismaru, M. (2020). Preventing youth from driving high. In: Canadian Journal of Family and Youth, vol. 12, nr. 1, p. 44-64.
[52]. Brookhuis, K.A., De Waard, D., Steyvers, F.J.J.M. & Bijsterveld, H. (2011). Let them experience a ride under the influence of alcohol; A successful intervention program? In: Accident Analysis & Prevention, vol. 43, nr. 3, p. 906-910.
[53]. Dobri, S.C.D., Moslehi, A.H. & Davies, T.C. (2019). Are oral fluid testing devices effective for the roadside detection of recent cannabis use? A systematic review. In: Public Health, vol. 171, p. 57-65.
[54]. Talpins, S.K., Holmes, E., Kelley-Baker, T., Walls, H.C., et al. (2017). Breath testing for cannabis: An emerging tool with great potential for law enforcement. National Traffic Law Center, Alexandria, VA.
[55]. Ullah, S., Sandqvist, S. & Beck, O. (2018). A liquid chromatography and tandem mass spectrometry method to determine 28 non-volatile drugs of abuse in exhaled breath. In: Journal of Pharmaceutical and Biomedical Analysis, vol. 148, p. 251-258.
[56]. Monteiro, S.P. (2014). Driving-impairing medicines and traffic safety; patients’ perspectives. PhD Thesis Groningen University, Groningen.
[57]. Emich, B., Van Dijk, L., Monteiro, S.P. & De Gier, J.J. (2014). A study comparing the effectiveness of three warning labels on the package of driving-impairing medicines. In: International Journal of Clinical Pharmacy, vol. 36, nr. 6, p. 1152-1159.
[58]. Ivers, T. & White, N.D. (2016). Potentially driver-impairing medications: Risks and strategies for injury prevention. In: American journal of lifestyle medicine, vol. 10, nr. 1, p. 17-20.
[59]. Nabben, T., Van der Pol, P. & Korf, D.J. (2017). Roes met een luchtje. Gebruik, gebruikers en markt van lachgas. Rozenberg Publishers, Amsterdam.
[60]. Camden, M.C., Hickman, J.S. & Hanowski, R.J. (2019). Effective strategies to improve safety case studies of commercial motor carrier safety advancement. National Surface Transportation Center for Excellence, Blacksburg, Virgina.
[61]. VNO-NCW & MKB-Nederland (2018). Werkgevers in verantwoordelijkheden beperkt door Autoriteit Persoonsgegevens, brief aan de VC's voor Justitie en Veiligheid en van SZW van de Tweede Kamer. Retrieved on 13-08-2019 at www.vno-ncw.nl/brieven-en-commentaren/werkgevers-verantwoordelijkheden-beperkt-door-autoriteit-persoonsgegevens.

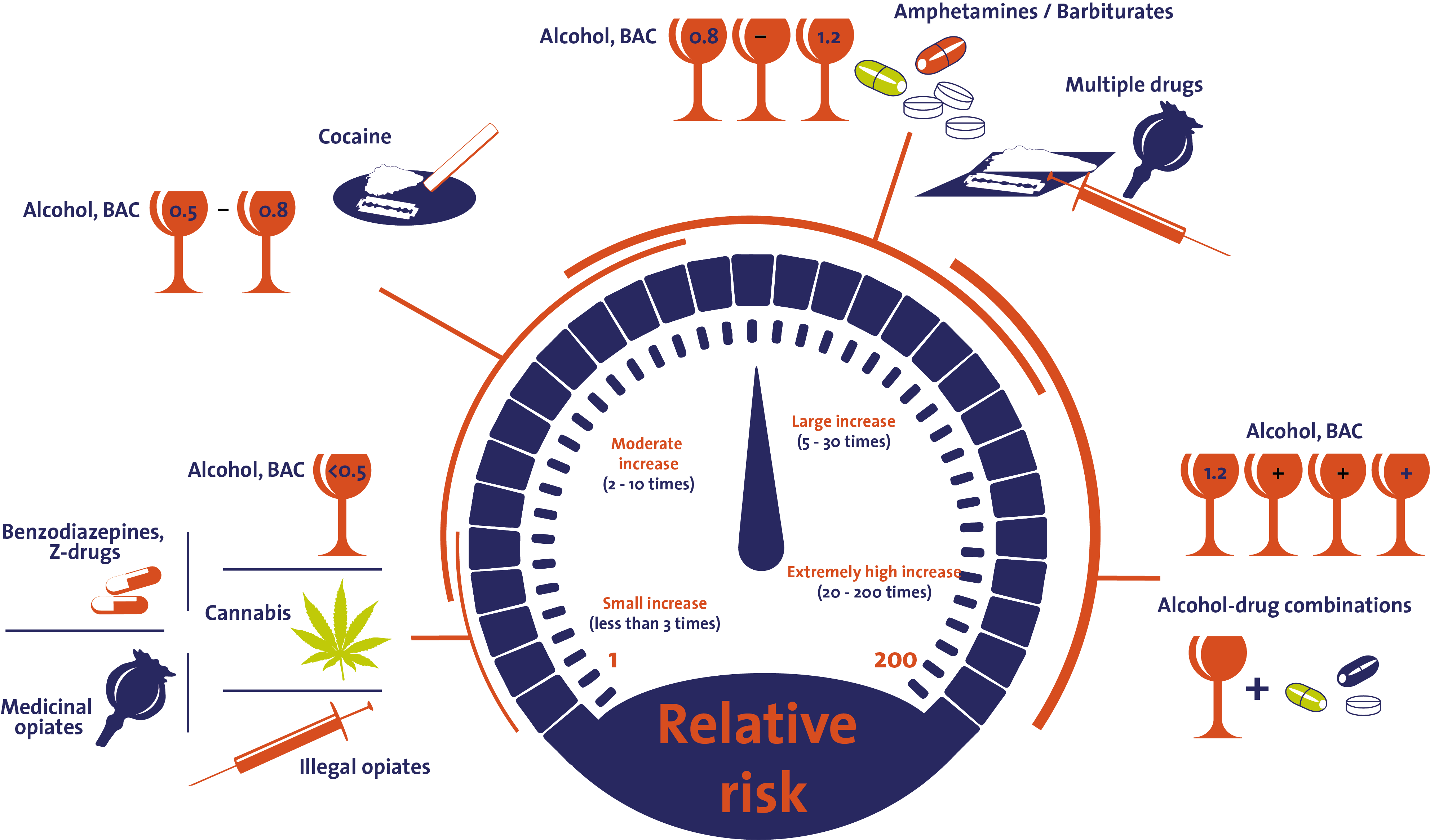 Figure 1. Schematic representation of the traffic risk attached to different drugs, medicines and alcohol (or combinations thereof) expressed in odds ratio’s
Figure 1. Schematic representation of the traffic risk attached to different drugs, medicines and alcohol (or combinations thereof) expressed in odds ratio’s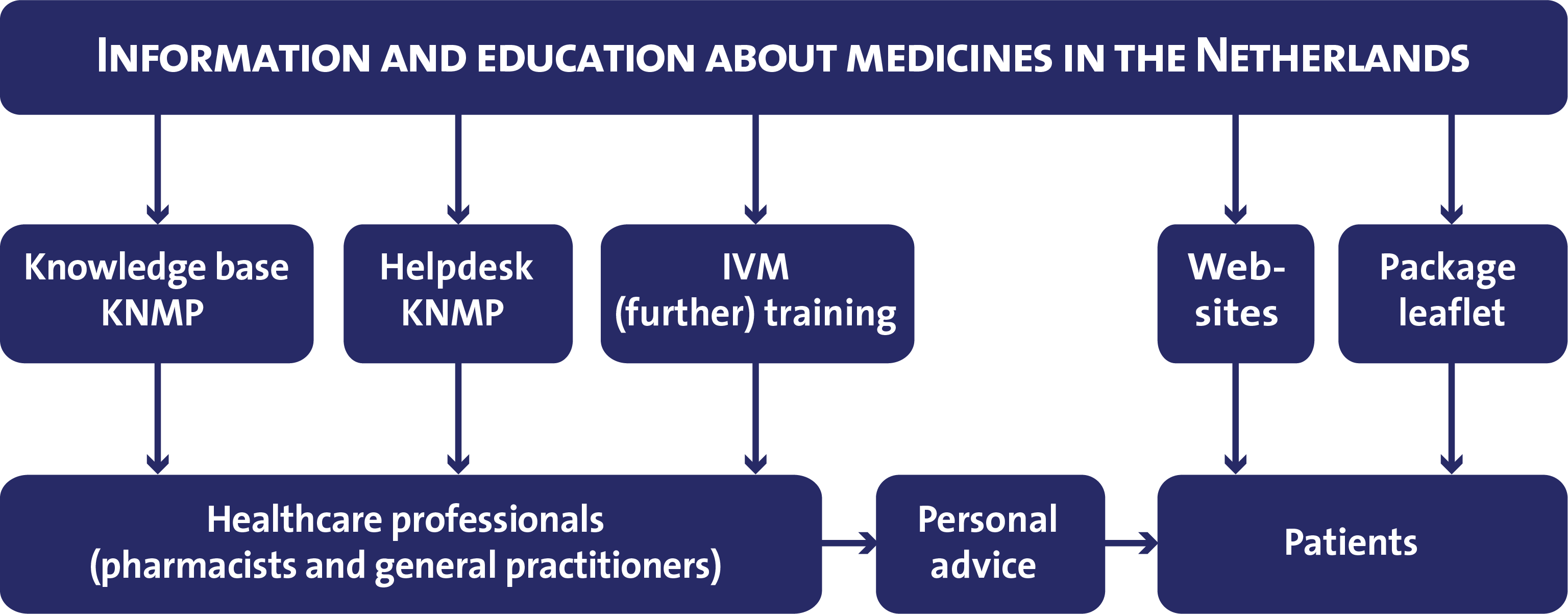 Figure 2. Information and education about medicines in the Netherlands: channels and target groups (KNMP = Koninklijke Nederlandse Maatschappij ter bevordering der Pharmacie (Pharmacists Association), IVM = Instituut Verantwoord Medicijngebruik (Dutch Institute for Rational Use of Medicine)).
Figure 2. Information and education about medicines in the Netherlands: channels and target groups (KNMP = Koninklijke Nederlandse Maatschappij ter bevordering der Pharmacie (Pharmacists Association), IVM = Instituut Verantwoord Medicijngebruik (Dutch Institute for Rational Use of Medicine)).